Implant dentistry in patients with bone loss can feel unfair and exhausting. You may hear mixed opinions. One dentist says no. Another suggests a risky fix. You need clear answers. Bone loss does not always end your chances for stable teeth. It does change the plan. You face higher costs, longer healing, and more visits. You also face more stress. Careful steps can lower that burden. You need a team that studies your medical history, scans your jaw, and explains limits and choices. Some patients need bone grafts. Some need shorter implants. Others need a Surprise prosthodontist who can rebuild a mouth that seems beyond repair. You deserve honest talk about risks, function, and time. This blog explains how experts manage complex cases so you can protect your health, control your expectations, and decide what feels right for your life.
Why bone loss changes your implant plan
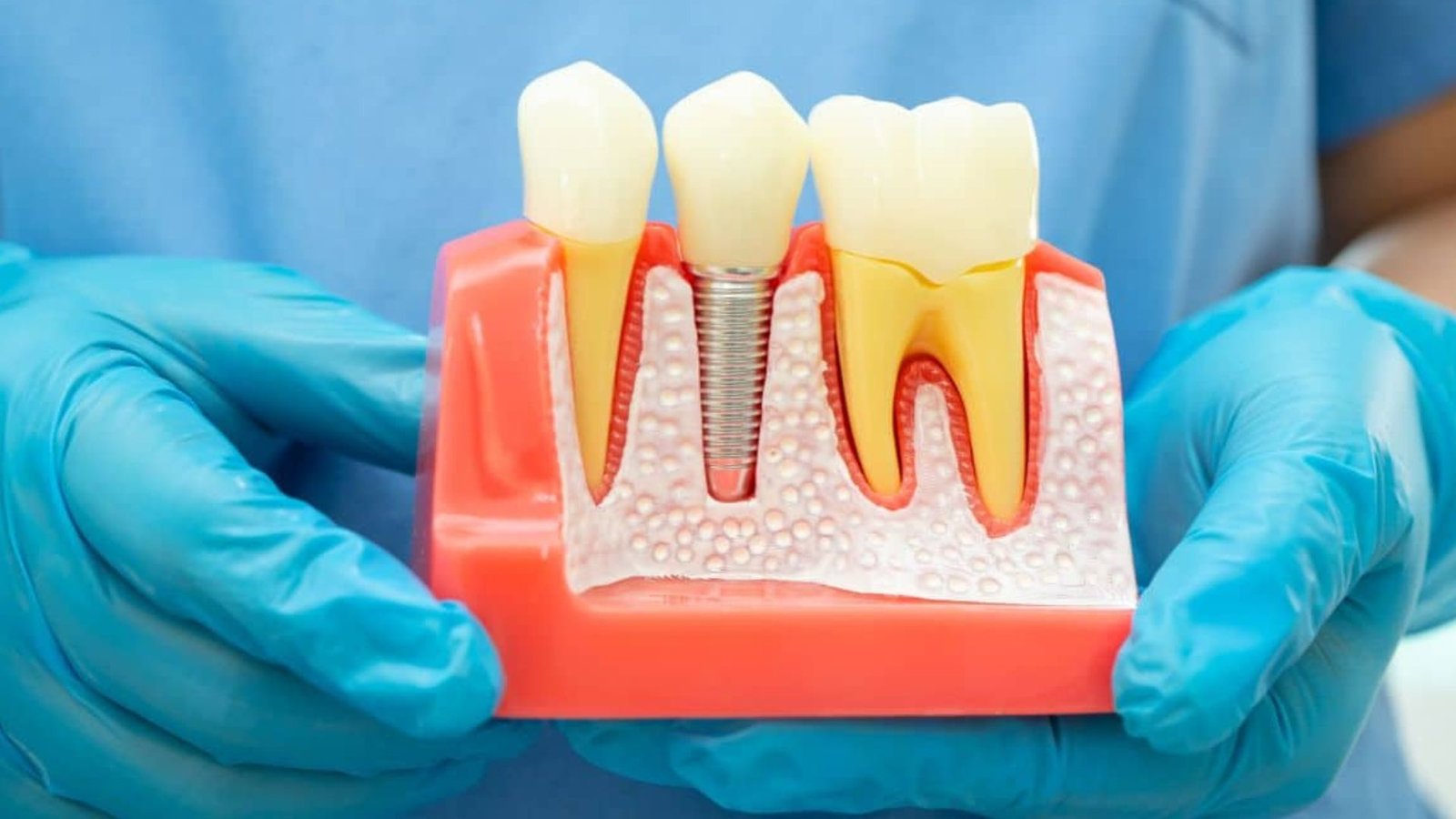
Bone holds each implant in place. When that support thins, the screw that acts like a root can loosen, fail, or harm nearby teeth and nerves. You may have bone loss from gum disease, missing teeth, infection, or long term denture use. You may also have health problems that slow healing. Each factor changes what is safe.
Your team looks at three simple questions.
- How much bone is left
- Where the bone sits
- How strong that bone is
Then your team matches the answers with your goals. You may want fixed teeth you never remove. You may accept a removable option if it protects your health. Clear talk about tradeoffs gives you control.
Also Read : 6 Common Dental Treatments Available In A Family Practice
Step one: testing and planning
The first visit should feel like a careful review, not a quick sales pitch. You can expect these steps.
- Medical history review for heart disease, diabetes, bone drugs, or smoking
- Head and neck exam to check gums, bite, and jaw joints
- 3D scan to measure bone height and width
- Review of medicines and allergies
- Discussion of your goals, fears, and budget limits
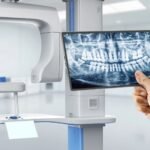
Accurate imaging matters. A National Institute of Dental and Craniofacial Research dental implant guide explains how jawbone health affects long-term success. Clear pictures help your team avoid nerves and sinus issues and choose implant sizes that match your bone.
Also Read : How Orthodontic Services Support Better Speech And Chewing
Common treatment paths for bone loss
Not every patient needs the same path. Here are three common options.
| Treatment choice | When used | Main pros | Main limits
|
|---|---|---|---|
| Bone graft with standard implants | Moderate to severe bone loss | Can restore support. Can allow standard implant sizes. | Higher cost. Longer healing. Extra surgery. |
| Short or narrow implants | Mild to moderate bone loss | Less surgery. Often shorter healing. | May not work for heavy bite forces. Not for every site. |
| Implant supported dentures | Many missing teeth or very thin bone | Better hold than regular dentures. Often fewer implants. | Still removable. Needs ongoing care and checks. |
Your team may also suggest staged care. First, they treat gum disease or infection. Then they place grafts or implants only after your mouth calms.
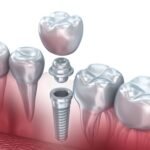
How bone grafts work
Bone grafts add or support bone so an implant has a stronger base. Your dentist may place graft material from your own body, a donor source, or a lab source. Your body then grows new bone around it.
Common graft types include these.
- Socket graft after a tooth comes out to slow bone loss
- Ridge graft to widen thin bone along the jaw
- Sinus lift to raise bone height in the upper back jaw
Healing can take months. That wait can feel hard. Yet strong bone lowers your risk of failure and repeat surgery. Honest talk about timeframes helps you plan work, school, and care tasks at home.
Risks you should know about
Every surgery has risks. Bone loss adds more. Clear consent means you hear these risks in plain words.
- Implant not bonding to bone
- Infection that needs cleaning or removal
- Nerve injury that can cause numbness or burning
- Sinus problems for upper implants
- Graft not healing as planned
Some health issues raise these risks. These include poorly controlled diabetes, immune conditions, strong bone drugs, or heavy tobacco use. The Centers for Disease Control and Prevention’s oral health page explains how long-term health and oral health connect. Sharing full medical details gives your team a chance to adapt your plan and lower harm.
Daily life with implants after bone loss
Implants can feel like a fresh start. Still, they are not “set and forget.” You protect your result with three steady habits.
- Brush twice each day with a soft brush and low foam paste
- Clean between implants and under bridges with floss, small brushes, or a water cleaner
- Keep regular checks and cleanings even when nothing hurts
You may also need a night guard if you grind your teeth. You may need stop smoking support. You may need help with blood sugar control. Small changes protect the bone you have left and the bone you gained.
Questions to ask your team
Strong decisions start with strong questions. You can bring this list to your visit.
- How much bone do I have in each planned site
- What are my top three options and why
- What happens if I do nothing for now
- How long will each step take from start to finish
- What problems should make me call you right away
- How many cases like mine do you treat each month
You deserve steady, patient answers. You also deserve time to think before you sign up for surgery.
Taking the next step
Bone loss makes implant care harder. It does not always make it impossible. Careful tests, honest talk, and a clear plan can turn a frightening choice into a managed one. You can ask for second opinions. You can slow the process until you feel ready. Your mouth carries your words, your food, and your smile. You deserve treatment that respects your weight and protects your health for the long term.